| Table of Contents |  |
|
Case Report
| ||||||
| Thoracoabdominal aortic aneurysm as a primary cause for mesenteric ischemia: A case report | ||||||
| William A. H. Maclean1, Ian M. Nordon2 | ||||||
|
1Surgical Trainee, Cardiovascular & Thoracic Division, University Hospital, Southampton NHS Foundation Trust, Tremona Road, Southampton, Hampshire SO16 6YD, United Kingdom.
2Vascular Consultant Surgeon, Cardiovascular & Thoracic Division University Hospital Southampton NHS Foundation Trust, Tremona Road, Southampton, Hampshire, SO16 6YD, United Kingdom. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Maclean WAH, Nordon IM. Thoracoabdominal aortic aneurysm as a primary cause for mesenteric ischemia: A case report. Edorium J Cardiothorac Vasc Surg 2015;2:1–3. |
|
Abstract
|
|
The majority of aortic aneurysms (AAs) are asymptomatic. As AAs expand they may become "symptomatic". This may be a consequence of local pressure effects. In the presence of a known AA, abdominal symptoms of pain, discomfort and bloating are often attributed to the known aneurysm, expediting the aneurysm treatment for fear of impending rupture. However, alternate diagnoses should be considered, these include diverticular disease, cholecystitis and retroperitoneal inflammation.
We report a case, a 70-year-old female presented with progressive epigastric and lower chest pain. This was subsequently confirmed to be as a result of acute mesenteric ischemia directly related to the progressive thrombus load within her thoracoabdominal aortic aneurysm and the atypical behaviour of this thrombus.
| |
|
Keywords:
Abdominal symptoms, Aortic aneurysm, Mesenteric ischemia, Thrombus
| |
|
Introduction
| ||||||
|
The majority of aortic aneurysms are asymptomatic. However, some may become "symptomatic" [1] which usually manifests as mild abdominal or back pain. In the presence of a known aneurysm this often expedites repair for fear of impending rupture. However, alternate diagnoses should be considered, these include diverticular disease, cholecystitis and retroperitoneal inflammation. We report a 70-year-old female presented with progressive epigastric and lower chest pain, which was subsequently confirmed to be due to acute mesenteric ischemia directly related to the unusual progressive thrombus load within her thoracoabdominal aortic aneurysm that was occluding the major branches. | ||||||
|
Case Report
| ||||||
|
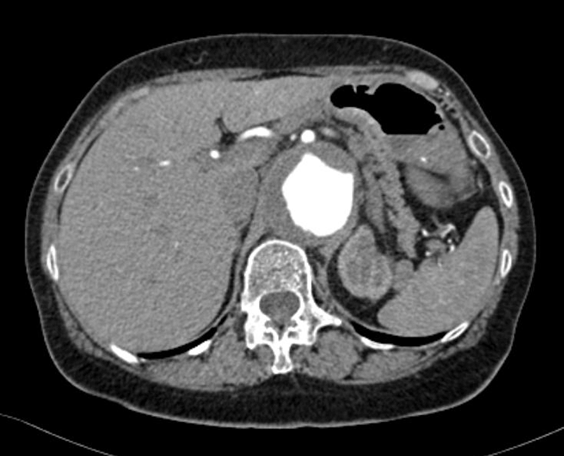
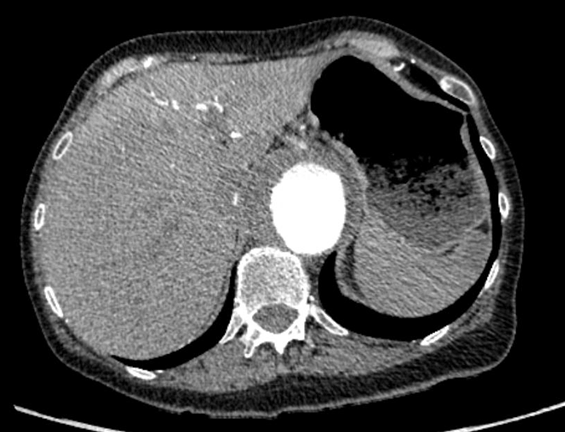
A 70-year-old female was seen on clinic in May 2013 for an asymptomatic aortic aneurysm discovered incidentally. This type IV thoracoabdominal aortic aneurysm extended from the distal thoracic aorta to the aortic bifurcation measuring 6.1 cm in its maximal diameter. She had a past medical history of polymyalgia rheumatica (on low dose prednisolone), three previous duodenal ulcers which were treated non-operatively, osteoporosis and osteoarthritis. Echocardiogram and ECG were within normal limits. She was worked up for elective open aortic repair as the aneurysm was not amenable to endovascular repair. However, one week prior to her planned surgery in August 2013, she was admitted under the cardiothoracic surgeons due to new and progressive epigastric and central lower chest pain radiating through to her back. She reported nausea, vomiting and anorexia. Clinical examination revealed normal observations. She had a clear chest on auscultation and there was a palpable aneurysm with local tenderness in the epigastric region. There was no evidence of peripheral vascular disease and all distal pulses were palpable. A FAST scan was performed in the emergency department on admission, which noted the aneurysm, but no free fluid to suggest any leak. Admission blood tests revealed mildly raised inflammatory markers (WCC 14.5 and CRP 18), other bloods were within normal limits. A computed tomograhpy (CT) scan angiography was booked and she was scheduled for the next elective list. In hospital, her symptoms deteriorated over two days from admission and her abdominal pain was exacerbated by eating. A CT angiography was performed on the morning of her second day of admission revealing the aneurysm had grown to 6.5 cm in maximum diameter, but excluded rupture or dissection. However, there was evident occlusion of the superior mesenteric artery (SMA) and coeliac axis secondary to the mural thrombus lining the anterior aspect of the aneurysm (Figure 1). Acute clinical deterioration occurred. Her lactate climbed to 6.3 from normal and she developed peritonitis, which was noted on the second night after admission. She was consented for an urgent exploratory laparotomy. At surgery, she was found to have irreversible bowel ischemia and an ischemic liver. A resection of the entire jejunum down to the ascending colon was completed. Retrograde revascularization was performed to both the superior mesenteric artery (SMA) and coeliac artery from her right common iliac artery using a long saphenous vein (Figure 2). On intensive care she continued to deteriorate. She was palliated and died two days after the surgery. | ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
This is the first case to report mesenteric ischemia as a result of organized aneurysm thrombus occluding the mesenteric visceral ostia. However, we suspect that this syndrome may well have occurred previously and labeled with an alternate diagnosis. This case raises a number of important issues related to misdiagnosis of "symptomatic" aneurysms, and gives new insight into the behaviour of aneurysm thrombus. The majority of aneurysms are lined with thrombus. This thrombus is thought to be a key factor in aneurysm progression due to the inflammatory mediators released from it [2]. When it comes to repair aneurysms by endovascular means, it is generally recognized as a safe technique to use a branched or fenestrated graft to accommodate visceral branches in the abdomen [3]. Multilayered stents are now being developed, which uses the theory that thrombus formation invariably maintains visceral vessel perfusion, thus the patency of the stent allows blood flow into these branches without complex placement of fenestration or bespoke branches [4]. Distal embolization of intra-luminal thrombus is a well-recognized phenomenon. However, as we demonstrate in this case, the organized intra-luminal thrombus may occlude the visceral vessels causing mesenteric ischemia and death. | ||||||
|
Conclusion
| ||||||
|
A patient with new abdominal pain and an unruptured abdominal aortic aneurysm should be considered very carefully. All alternate diagnoses unrelated to the aneurysm should be explored and common diseases such as cholecystitis or diverticulitis need to be excluded. This case highlights the fact that this search for an alternate diagnosis should be exhaustive and expedited including mesenteric ischemia. If diagnosis is delayed then irreversible bowel necrosis can occur in the presence of two treatable pathologies. It also demonstrates new insight into abnormal thrombus behavior and could impact on our theory behind new graft technology. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
William A. H. Maclean – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Ian M. Nordon – Substantial contributions to conception and design, Acquisition of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 William A. H. Maclean et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|